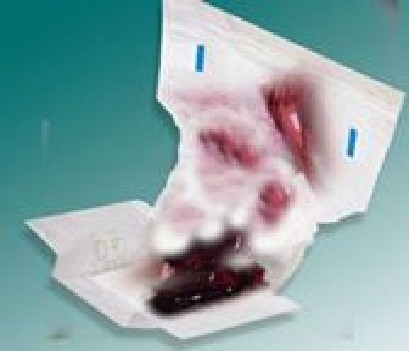
A 6-month-old infant is seen in the ED. The mother claims that the child was being breastfed when he suddenly started to cry and refused feedings. The child became extremely irritable, pale and had one episode of non-bilious vomiting. There is no other past significant history. The child is up to date on his vaccines. He recently had a URTI that was treated conservatively. The examination reveals a tense abdomen. You open the diaper and see the following (see image below). What is the next step in the management of this infant?
A. Obtain Ultrasound of the abdomen
B. Check stools for ova and parasites
C. Tell radiologist to insufflate the colon with air at 50-100 mmHg
D. Perform flexible sigmoidoscopy
E. Prepare infant for laparoscopic surgery
-
The appearance of maroon-colored stools and the history are classic for intussusception.
-
Unless the child has obvious signs of peritonitis, the standard of care is air or barium enema to reduce the intussusception
-
The air pressure should not be more than 110 mmHg.
-
If contrast is used, the column should be at 3 feet maximum and one should not make more than 3 attempts
-
Post-reduction images are mandatory to determine if the reduction is successful
-
Only delayed cases need surgery