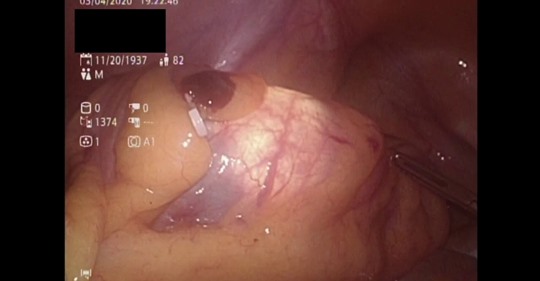
A case of an 82 y/o Filipino gentleman, pmhx of HTN, hyperlipidemia, CKD, came in for PR bleeding. Colonoscopy showed Sigmoid Ca 30 cm FAV. After careful discussion, patient refused CT AP in view of high risk contrast-induced nephropathy (thoughts?). For what it’s worth, the Liver USG, CXR and CEA were all normal. After informed consent, decision made for Laparoscopic High AR/Sigmoidectomy with ICG KIV intraop colonoscopy (for tumor localization). Straight forward case really, except that somehow the planes seemed to be ‘stickier’ than usual (or is it just me). We did proceed with the introp colonoscopy for precise tumor localization since preoperative endoscopic tattooing was not done ( although the tumor seemed to be ‘palpable’ during laparoscopy - I just felt the need to confirm it with endoscopy (‘kiasu’ - took my fellowship in Singapore, go figure). Finally, you cannot really be too careful in dealing with these patient population (elderly, ?Sudeck’s point esp. after high IMA ligation), so apart from our routine air insufflation and endoscopic visualization, we utilized ICG-enhanced Fluorescence Imaging to asses anastomotic tissue perfusion. It’s safe (remove from the circulation exclusively by the liver - no metabolism and eliminated by active diffusion ), easy to perform and adds little to the operating time. Our patient did well post-op under ERAS protocol. He was discharged post-op day 3.